Semen quality is one of the main indicators of general male reproductive health and fertility. In recent decades the change in semen quality has attracted interest from researchers wishing to explore the possible risk factors and determinants (1). Great attention was paid to the effect of environmental hazards, chemicals, occupational hazards and physical factors.
In recent years, social factors, psychological factors and behaviours/lifestyles have become increasingly important health determinants. However, the impact of these factors on semen quality is unclear (1).
Scientific Evidence on Underwear Type and Sperm Quality
In specialized bibliography, there are some studies that conclude with no relationship between the type of underwear and sperm quality (2, 8, 9).
On the other hand, we also find studies that conclude that the type of underwear can influence in sperm quality (1, 3, 4, 5, 6, 7).
Impact of Synthetic Fabrics and Underwear Materials
Related to this, research in semen samples from 1346 healthy men conclude that semen quality can be impacted by wearing manmade fibre underwear (1). They did not observe that wearing tight-fitting underwear was significantly associated with semen quality but did find that wearing fibre underwear often lowered the percentage of normal sperm morphology (p=0.001). Generally speaking, the constituent material of fibre underwear contains chemical substances (such as formaldehyde resin and anti-wrinkle treatment agents) and assists urethra bacterial growth and reproduction due to poor sweat absorption. This may be one explanation for the decreased normal sperm morphology observed in men who wore fibre underwear (1).
Testicular Heat and Its Effect on Sperm Quality
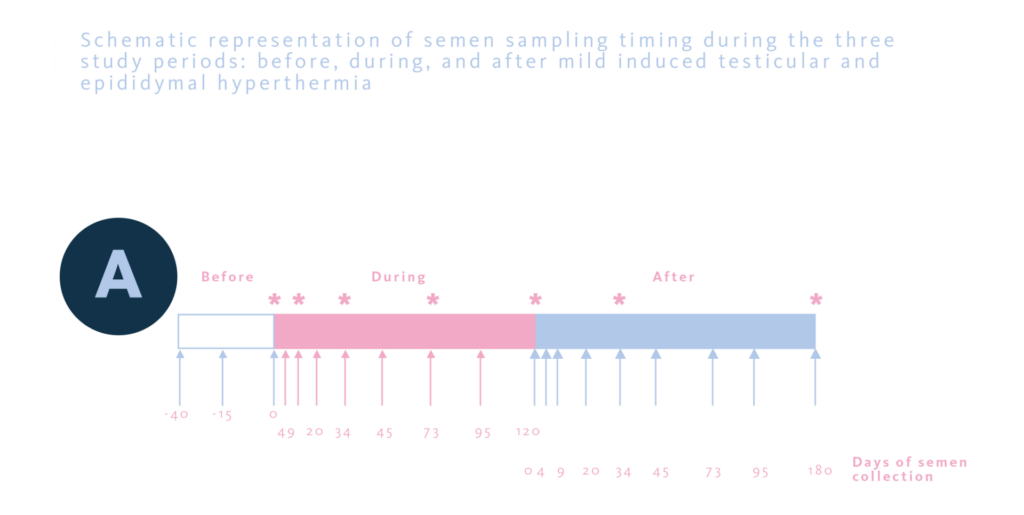
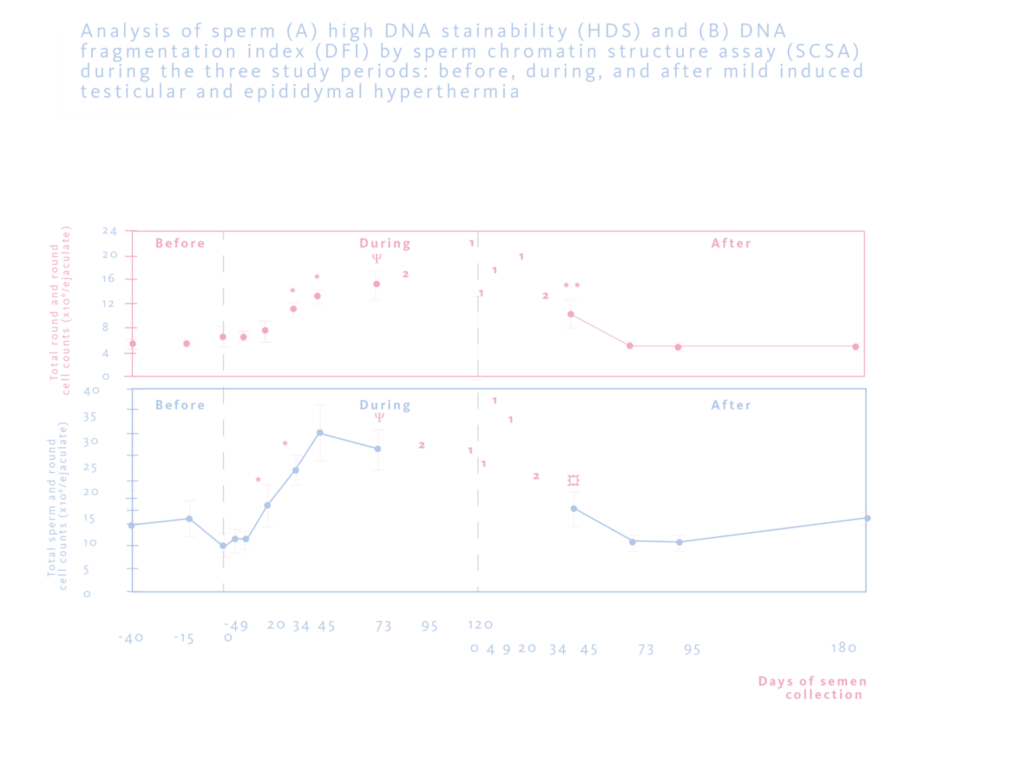
To investigate the effects of a mild induced testicular and epididymal hyperthermia (+2ºC) on sperm chromatin integrity, five healthy fertile volunteer men were subjected to an a experimental prospective study. In this way, testicular and epididymal hyperthermia was induced by maintaining the testes at inguinal position with the support of specially designed underwear 15 hours daily for 120 consecutive days. Classic semen characteristics, sperm DNA fragmentation index (DFI) and high DNA stainability (HDS) were analyzed by sperm chromatin structure assay(3).
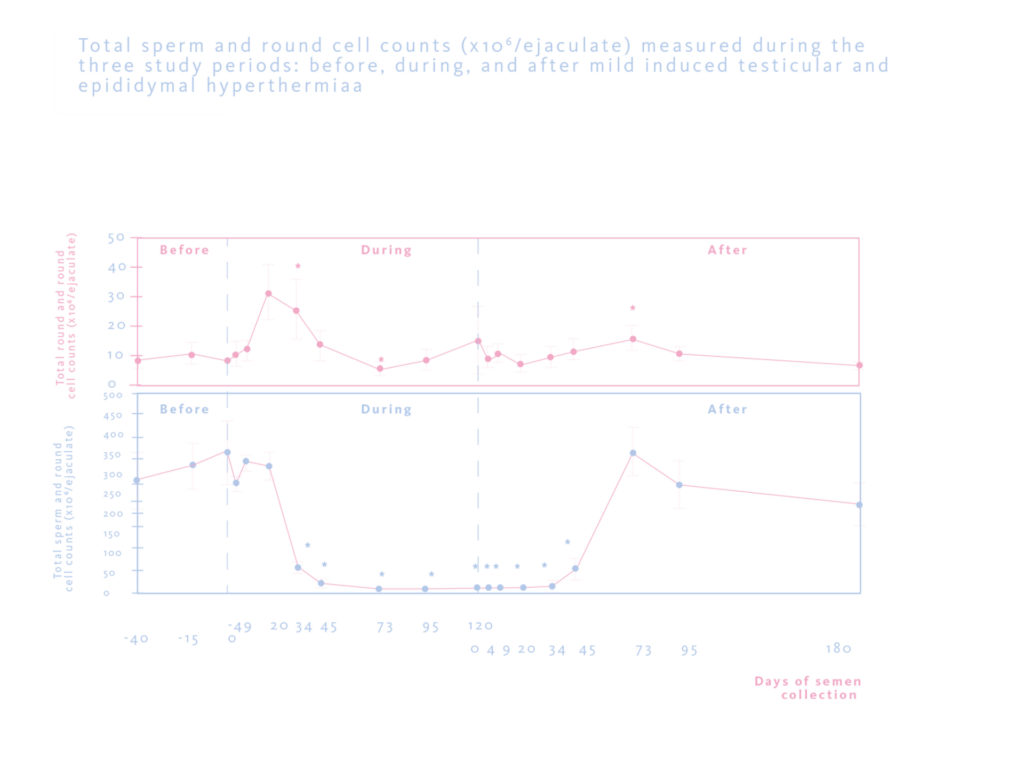
In the results, compared with baseline values, sperm DFI and HDS were significantly increased as early as day (D) 20 and D34, respectively, and remained elevated during the entire period of hyperthermia. Percentages of motile and viable spermatozoa decreased as early as D20 and D34, respectively, and total sperm count decreased at D34 during hyperthermia and remained low during the entire hyperthermia period. All studied parameters returned to respective baseline values at D73 after cessation of hyperthermia.
In conclusion, mild induced testicular and epididymal hyperthermia largely impaired sperm chromatin integrity, which appeared before any changes in sperm output. These findings may have clinical implications in male contraception, infertility, and assisted reproductive technology(3). Similar results were observed in (4) and (5).
Lifestyle Factors and Sperm Aneuploidy
The aim of another study (6) was to examine the association between lifestyle factors and sperm aneuploidy. The study population consisted of 212 healthy men under 45 years of age attending an infertility clinic for diagnostic purposes and who had a normal semen concentration of 20– 300 x 106/mL or slight oligozoospermia (semen concentration of 15–20 106/mL). All participants were interviewed and provided a semen sample. Sperm aneuploidy was assessed using multicolor FISH (DNA probes specific for chromosomes X, Y, 18, 13, 21).
Results from the study suggest that lifestyle factors are related to sperm aneuploidy. In this sense, the results demonstrated a significant relationship between wearing boxer shorts and sperm aneuploidy (lack of chromosome XY or 13, additional chromosome 18 or 21 and complex copy changes in the whole chromosome 18) (6).
In the study of Kaya in 2020 (7), 1311 participants who attended the Andrology Clinic were separated into two groups as men with normozoospermia and dysspermia. All participants answered a questionnaire which contains questions about the modifiable lifestyle factors. In the results, a negative relationship between the wearing of tight underwear and having normal semen parameters. Wearing tight underwear was related to both lower motility, normal morphology as well as semen concentration (p < 0.05) (7).
Studies Showing No Relationship Between Underwear and Fertility
We can also find studies that conclude there is no relationship between the type of underwear and semen quality.
Related to this, the modifiable and non-modifiable risk factors for poor sperm morphology were analyzed in a multi-centre case-referent study in which cases (<4% normal morphology forms) and referents (> 4% normal morphology forms) were male patients identified at their first visit to either a fertility or gynaecology clinic or to an andrology laboratory for semen analysis or when a first appointment was made for a semen analysis (8). Men aged 18 years or above were recruited from 14 fertility clinics across the UK during a 37-month period (8).
They also had to have no knowledge of the result of any previous semen analysis. this criterion was included to remove the possibility of bias in response to questions on exposures and risk factors. In their conclusions, no significant association was found between type of underwear and sperm morphology (8).
Another study try to investigate the relationship between male underwear-type worn during daytime/bedtime and male fecundity as measured by semen quality and time-to-pregnancy (9). 501 Couples were enrolled and followed for 12 months. Male partners provided semen samples that were analyzed for 35 semen quality endpoints. At enrollment, men provided information on type of underwear worn during daytime and bedtime and were classified into 6 categories by underwear choice (n = 491) (9).
The autors don´t find any significant differences in time-to-pregnancy, conception delay or infertility, by underwear type. So, they conclude that the style of the male partner’s underwear does not seem to affect a couple’s ability to achieve pregnancy (9).
Conclusions
The bibliography consulted shows that there is controversy as to whether the type of male underwear can, or cannot, influence semen quality.
However, considering that there are more publications that support the idea that the type of men’s underwear influences semen quality, we can reach the same conclusion.
Anyway, the fact that there are publications that disagree with this conclusion makes it necessary to have a greater number of studies that analyze men’s lifestyle habits correctly from the point of view of evidence-based medicine.
BIBLIOGRAPHY
1. Li Y, Li Y, Zhou N, et al. Socio-psycho-behavioural factors associated with male semen quality in China: results from 1346 healthy men in Chongqing. J. of Family Planning and Reprod. Health Care. 2013; 39: 102–110.
2. Oldereid NB, Rui H and Purvis K. Lifestyles of men in barren couples and their relationships to sperm quality. Europ. J. of Obstet. & Gynecol. and Reprod. Biology. 1992; 43: 51-57.
3. Ahmad G, Moinard N, et al. Mild induced testicular and epididymal hyperthermia alters sperm chromatin integrity in men. Fertil. and Steril. 2012; 97(3): 546-553.
4. Abdelhamid MHM, Walschaerts M, et al. Mild experimental increase in testis and epididymis temperature in men: effects on sperm morphology according to spermatogenesis stages. Transl. Androl. Urol. 2019; 8(6): 651-665. (doi: 10.21037/tau.2019.11.18).
5. Abdelhamid MHM, Esquerre-Lamare C, et al. Experimental mild increase in testicular temperature has drastic, but reversible, effect on sperm aneuploidy in men: A pilot study Reprod. Biol. 2019; 19: 189-194. (doi.org/10.1016/j.repbio.2019.06.001).
6. Jurewicz J, Radwan M, et al. Lifestyle factors and sperm aneuploidy. Reprod. Biol. 2014; 14(3): 190-199. (doi.org/10.1016/j. repbio.2014.02.002).
7. Kaya C, Aykaç A et al. The effect of modifiable lifestyle factors on semen quality. Rev. Int. of Androl. 2020; 18(4): 151-158. (doi.org/10.1016/j.androl.2019.09.001).
8. Pacey AA, Povey AC, et al. Modifiable and non-modifiable risk factors for poor sperm morphology. Hum. Rep. 2014; 29(8): 1629-1636. (doi:10.1093/humrep/deu116).
9. Sapra KJ, Eisenberg ML, et al. Choice of underwear and male fecundity in a preconception cohort of couples. Andrology. 2016; 4(3): 500-508. (doi:10.1111/andr.12163).