In a recent study published in Nature Scientific Reports, researchers investigated whether the use of electronic cigarettes affects semen quality and live birth outcomes differently compared to traditional cigarette smoking in couples undergoing assisted reproductive treatment.
The findings revealed a higher live birth rate and improved sperm motility in the vaping group compared to those who smoked conventional cigarettes. Interestingly, however, sperm concentration was found to be higher among traditional cigarette users.
One notable limitation of the study is the absence of a non-smoking control group. Without this comparison, it remains difficult to fully understand the impact of vaping on male fertility in the context of IVF.
Background
Tobacco use remains one of the greatest public health challenges worldwide. Each year, it causes over 7 million deaths, along with long-term disability and suffering from tobacco-related diseases. Fortunately, traditional cigarette smoking has been steadily declining: according to the World Health Organisation (WHO), global smoking rates have dropped from 33% in 2000 to 20% in 2024.
Despite decades of awareness campaigns, around one-third of men of reproductive age still smoke traditional cigarettes. Meanwhile, e-cigarettes, sleek devices that vaporise flavoured nicotine liquids, have surged in popularity, especially among younger populations. Although often marketed as a safer alternative, the long-term health effects of these products remain largely unknown.
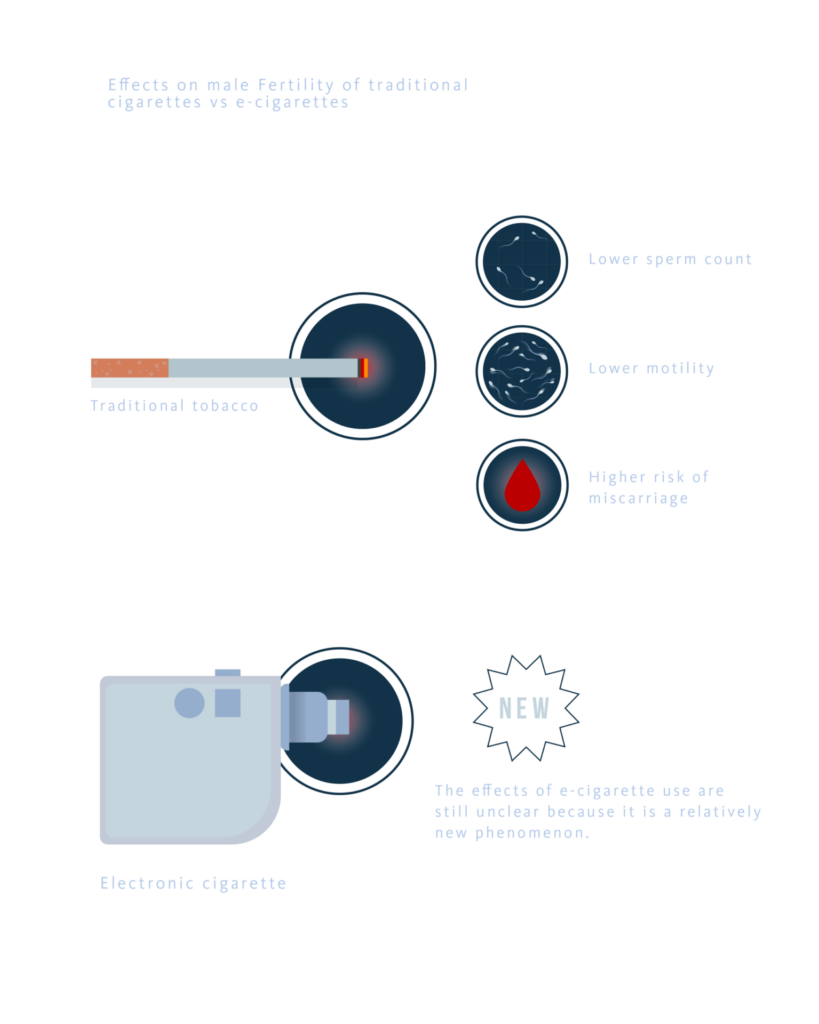
Smoking conventional cigarettes is strongly associated with male fertility issues, including lower sperm counts, reduced motility, and an increased risk of miscarriage in partners. In contrast, the effects of vaping remain less well understood. Although e-cigarette aerosols contain harmful substances such as metals and aldehydes, their specific impact on reproductive health has yet to be clearly defined.
About the study
Medical records from 296 South Korean couples who underwent in vitro fertilisation (IVF) or intracytoplasmic sperm injection (ICSI) were analysed. Male partners had exclusively smoked either conventional cigarettes or e-cigarettes for at least six months, while all female partners were non-smokers.
Only women diagnosed with tubal disease, polycystic ovary syndrome (PCOS), thyroid dysfunction, hyperprolactinemia, or with a history of failed intrauterine insemination were included in the study. Men with significant medical histories or previously documented abnormal semen analyses were excluded.
Before the IVF cycle, researchers conducted a standard semen analysis, calculated body mass index (BMI), and measured serum levels of follicle-stimulating hormone (FSH), luteinizing hormone (LH), testosterone, prolactin, anti-Müllerian hormone (AMH), and sex hormone-binding globulin (SHBG). Controlled ovarian stimulation was carried out using a gonadotropin-releasing hormone (GnRH) antagonist protocol.
Oocyte retrieval was performed 36 hours after administration of a recombinant human chorionic gonadotropin (hCG) trigger. All embryos were cryopreserved at the blastocyst stage and transferred during frozen-thawed cycles. Study outcomes included semen parameters, pregnancy rates, miscarriage rates, and live birth rates.
Results
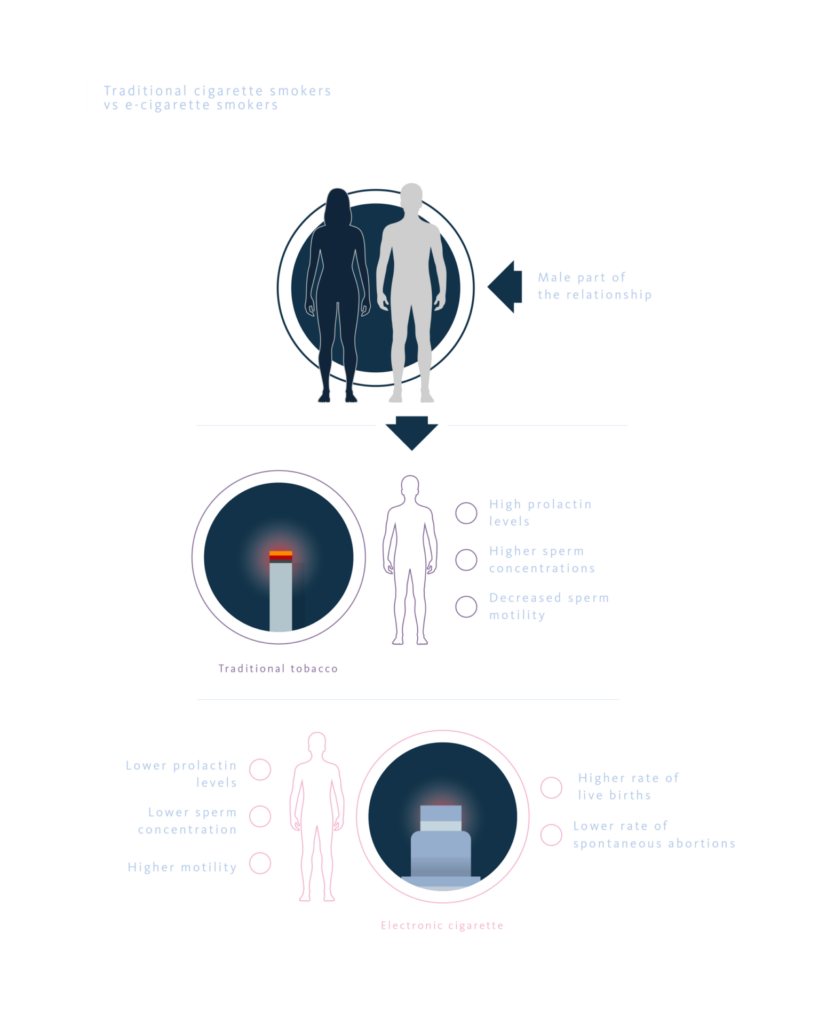
Among the 296 participants, traditional cigarette smokers (n=151) exhibited higher serum prolactin levels and greater sperm concentration, whereas progressive sperm motility was significantly higher among e-cigarette users (n=145). Other semen parameters showed no significant differences between the groups. Female partners in both cohorts were similar in age and ovarian reserve markers. Controlled ovarian stimulation protocols were applied uniformly, resulting in comparable numbers of oocytes retrieved and two-pronuclear (2PN) embryos. The only notable difference among female partners was body mass index (BMI), which was moderately higher in the group whose male partners smoked conventional cigarettes.
Importantly, the live birth rate was significantly higher in the e-cigarette group compared to the conventional cigarette group (56% vs. 41%). Additionally, the clinical miscarriage rate was markedly higher among couples where the male partner smoked traditional cigarettes (36% vs. 12%).
However, multivariable logistic regression analysis revealed that, although differences in semen parameters and live birth outcomes were observed between cigarette types, key predictors of live birth, such as follicle-stimulating hormone (FSH) levels and the number of two-pronuclear (2PN) embryos, did not differ significantly between the groups.
Conclusions
Vape use by male partners undergoing IVF appears to be less detrimental to reproductive success than continued use of conventional cigarettes. Although sperm concentration was slightly lower among vapers, they exhibited higher progressive motility and lower prolactin levels. These differences led to a significantly lower miscarriage rate and a notable 15-percentage-point increase in live birth rate compared to traditional smokers.
Importantly, the type of cigarette used did not outweigh established predictors such as FSH levels or embryo count, highlighting that vaping offers no guarantee of success.
This study presents several clear limitations, the most significant being the absence of a non-smoking control group. Including such a group would have allowed for a more accurate assessment of the true impact of e-cigarettes on male fertility. For this reason, the authors emphasise that these findings should not be interpreted as an endorsement of e-cigarette use. Vaping still carries potential health risks, and its long-term effects on reproductive health remain poorly understood. The current recommendation continues to be that abstaining from all forms of tobacco use is most beneficial for reproductive health.
References
- Kim, H. K., Choi, W. Y., Lee, J. I., & Kim, T. J. (2025). Impact of conventional cigarette and electronic cigarette use on sperm quality and IVF/ICSI outcomes. Scientific reports, 15(1), 23714. https://doi.org/10.1038/s41598-025-09495-w
- WHO global report on trends in prevalence of tobacco use 2000–2030. https://www.who.int/publications/i/item/9789240088283
- Sharma, R., Harlev, A., Agarwal, A., & Esteves, S. C. (2016). Cigarette Smoking and Semen Quality: A New Meta-analysis Examining the Effect of the 2010 World Health Organisation Laboratory Methods for the Examination of Human Semen. European urology, 70(4), 635–645. https://doi.org/10.1016/j.eururo.2016.04.010
